Our Publications
The New Consumer Protection Act Controversy: Does It Apply to Doctors in India?
A new Consumer Protection Act (CPA) was introduced in 2019 and has created quite a stir in the medical fraternity. There is widespread uncertainty as to whether this new Act applies to the medical profession. However, on careful review of the original CPA of 1986, the definition of services included within the Act, and understanding the changes introduced in CPA 2019, the legal application of CPA 2019 to medical professionals becomes clear. While the term medical services has been removed from the list of services under the purview of the Act, the phrase "but not limited to" before listing the services leaves the door open for the inclusion of other services.


In the Hands of a Robot, From the Operating Room to the Courtroom: The Medicolegal Considerations of Robotic Surgery
Robotic surgery has rapidly evolved as a groundbreaking field in medicine, revolutionizing surgical practices across various specialties. Despite its numerous benefits, the adoption of robotic surgery faces significant medicolegal challenges. This article delves into the underexplored legal implications of robotic surgery and identifies three distinct medicolegal problems. First, the lack of standardized training and credentialing for robotic surgery poses potential risks to patient safety and surgeon competence. Second, informed consent processes require additional considerations to ensure patients are fully aware of the technology's capabilities and potential risks. Finally, the issue of legal liability becomes complex due to the involvement of multiple stakeholders in the functioning of robotic systems. The article highlights the need for comprehensive guidelines, regulations, and training programs to navigate the medicolegal aspects of robotic surgery effectively, thereby unlocking its full potential for the future.
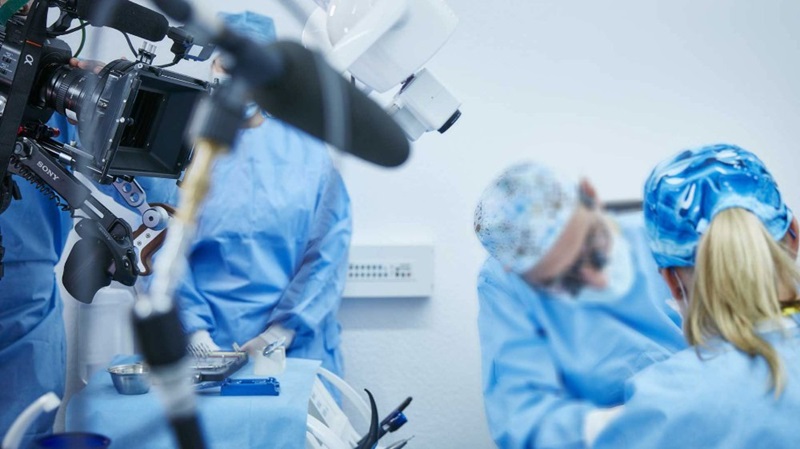
The Theatre of Surgery: The Ethical and Legal Implications of Live Surgeries
Surgical training has long emphasized learning through direct observation, allowing young surgeons to gain practical insights from experienced surgeons. The advent of live surgical demonstrations has extended this learning method, providing real-time broadcasts of surgeries to wider audiences. Live surgery is a surgery that is broadcasted in real time to an audience. While live surgeries offer substantial educational benefits, enabling the rapid dissemination of advanced surgical techniques and reducing the learning curve for surgeons, they also raise critical ethical and legal questions. Concerns include potential compromises in surgical outcomes due to increased pressure on surgeons, the ethical implications of patient consent, privacy issues, and the ambiguity of accountability when complications arise. In India, these concerns have intensified following a patient's death during a live surgery, prompting legal scrutiny and a Supreme Court petition seeking to regulate the practice. This article delves into the multifaceted debate surrounding live surgeries, examining both their educational value and the ethical, legal, and practical challenges they pose. We aim to provide a comprehensive overview that will inform readers about the complexities of live surgeries, spread awareness, and stimulate further discussions on this evolving practice.
The Witness to an Informed Consent for Surgery/Invasive Procedure: The Ethical and Legal Aspects
Informed consent is an exercise to protect the right of the patient to make an informed decision regarding his/her willingness to undergo a procedure. The doctor needs to explain all aspects of the procedure to the patient beforehand, including the nature of the procedure, its purpose, alternatives, and possible complications. The patient’s signature is required on a written informed consent to document their willingness for the procedure. It is required by law that such an informed consent be obtained from every patient undergoing any invasive procedure. However, the role of a witness for the informed consent is ambiguous. This brings up certain important questions regarding the witness for an informed consent – is it necessary? And if so, who should be a witness?


Swallowing the Litigation Pill: The Future of Medical Lawsuits in India
As the tide of medical lawsuits rises, doctors in India find themselves navigating increasingly treacherous waters. What drives this surge in litigation? Can we chart a course through these challenging times, or are we destined to face relentless legal battles? In this editorial, we unravel the complexities of this pressing issue and glimpse what lies on the horizon for India's medical community.


Understanding the Medico-Legal Aspects of Telemedicine in India
Telemedicine has brought a new dimension to healthcare and has been gaining popularity worldwide. However, the medico-legal aspects of the practice of telemedicine in India remain ambiguous to most doctors and administrators. We have therefore provided a concise overview of the legal aspects of telemedicine, which will enable doctors and administrators to provide better telemedicine services while safeguarding themselves from possible litigation.


Osteoporosis - An Imminent Ethical and Legal Debacle?
Osteoporosis is a condition characterized by a decrease in bone density. Its prevalence is on the rise and is only going to continue to rise further. Fragility fractures such as neck of femur fracture fractures and intertrochanteric fractures are among the most common fractures encountered by orthopedic surgeons today. Yet, the management of these fragility fractures has unfortunately fallen short of addressing the etiology behind the fracture. Orthopedic surgeons routinely perform arthroplasty or osteosynthesis for stabilization of these fractures, but rarely do they address the coexisting osteoporosis. We explore the factors, leading to this scenario, the practical hurdles faced, the ethical and legal considerations on the matter, and the road ahead. We believe that this is a topic which should be discussed further among orthopedic surgeons to arrive at practical solutions and change in perspectives. The aim of this article was to encourage a debate on the matter, increase awareness about the current situation, and help change the trend in the management of osteoporosis in developing countries like India.


The New Bharatiya Nyaya Sanhita Laws: Progress or Pitfall for Doctors?
The Indian Penal Code (IPC), a relic of British colonial rule, was recently replaced by the Bharatiya Nyaya Sanhita (BNS) in July 2024. While the overhaul of the IPC was largely welcomed, it has sparked significant concern among the medical community, primarily due to Section 106 of the BNS. This section mandates imprisonment for doctors involved in deaths caused by rash or negligent acts during medical procedures, which many in the profession fear could lead to a climate of fear and hesitancy in performing critical medical interventions. This article delves into the contentious aspects of the BNS, comparing them to the old IPC provisions and examining the specific fears and protests of medical professionals. It also explores the legal nuances and potential impacts on medical practice, aiming to provide a balanced perspective and foster informed discussions within the medical community. Through this examination, the article seeks to dispel unfounded fears, highlight the protective measures within the BNS, and propose constructive approaches to ensure fair assessment in medicolegal cases, ultimately advocating for a legal environment that supports rather than hinders the medical profession.


Medical Termination of Pregnancy Act of India: Treading the Path between Practical and Ethical Reproductive Justice
One of the most important facets of reproductive freedom and justice is the right to abortion. For centuries, the debate on legalisation and regulation of abortion has caused ethical dilemmas with proponents for both sides of the argument. India, a developing nation, with a wide spectrum of cultures, traditions, socio-economic statuses and religious beliefs, would be expected to be grappling with this problem. However, India since the 1970s made a clear stance on the matter of abortion. Respecting the right to personal liberty, reproductive freedom of women and upholding the importance of women's health, Medical Termination Pregnancy (MTP) has been legal in India since 1971. We look at the laws governing MTP in India, the practical and ethical considerations, the recent amendments in these laws and the road ahead.


Doctor, Bot, or Both: Questioning the Medicolegal Liability of Artificial Intelligence in Indian Healthcare
Artificial intelligence (AI) is rapidly transforming the landscape of healthcare, with its applications ranging from diagnostics to robotic surgery. As India swiftly integrates AI into its healthcare system, a critical question arises: who bears the liability when AI-driven medical decisions go wrong? This article explores the complexities of assigning legal responsibility for AI in healthcare, particularly within the Indian context. While India's legal framework, including the Information Technology Act, intersects with AI usage, it lacks specific provisions addressing AI liability. The National Strategy for AI, although a step forward, does not resolve the ambiguities surrounding accountability. The article also examines how other countries, particularly the European Union and the United States, are beginning to tackle these challenges through proposed directives and regulations. However, the absence of clear, comprehensive laws worldwide reflects the inherent difficulties in legislating AI stemming from its autonomous nature, the "black box" problem, and the multifaceted roles of stakeholders. Until robust legal frameworks are established, the article cautions healthcare professionals to exercise vigilance when using AI tools, recognizing that they may still bear significant liability. This evolving legal landscape underscores the need for continued deliberations in AI regulations.


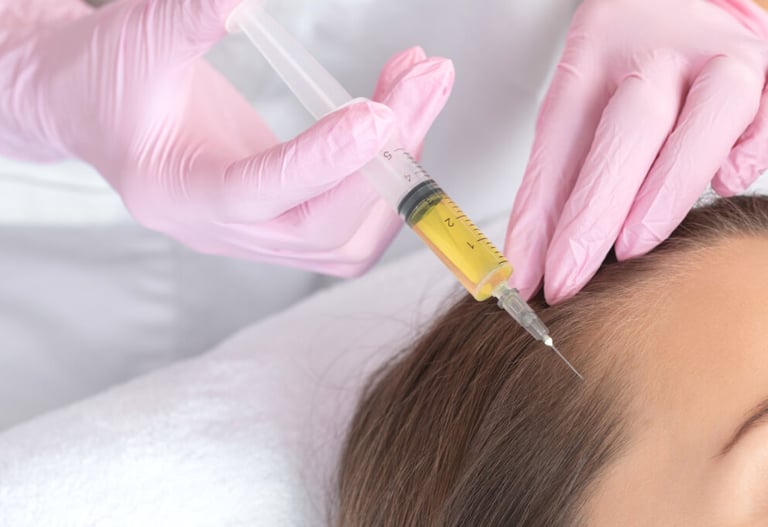
Standardized Informed Consent Form for Clinicians Administering Platelet-Rich Plasma
Introduction When it comes to medico-legal malpractice suits, lawyers and insurers tend to focus on informed consent documentation. Unfortunately, there is no standard protocol for obtaining informed consent for the use of platelet-rich plasma (PRP) injections, which might cause problems. This study aimed to mitigate this concern through the development of a standardized informed consent document for PRP injections, grounded in evidence-based practices. Materials and methods An examination of databases was conducted to explore the medico-legal ramifications associated with PRP injections, as well as the broader topic of informed consent, with a particular focus on the context of PRP injections. Moreover, interviews were carried out with healthcare providers and individuals who had received PRP injections within the preceding year, utilizing a semi-structured methodology. Results We developed an evidence-based informed consent document tailored for PRP injections. To guarantee its legal validity, the document underwent review by a legal specialist. Subsequently, our institutions implemented the finalized form for PRP injection procedures over one year. Conclusion A legally valid and evidence-based informed consent form for PRP injections would ensure patient's rights, and encourage open communication and transparency between them and the doctor. Moreover, if a lawsuit were to arise, it would serve as a critical document in the doctor's defense and withstand scrutiny from lawyers and the judiciary.
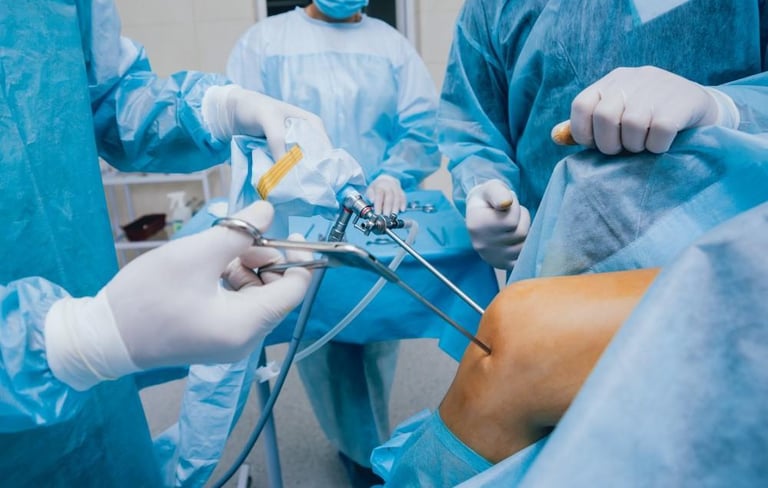
Arthroscopy in India Through the Medicolegal Lens: A Comprehensive Review
With the increasing number of Arthroscopic surgeries, comes with it, the undesirable problem of litigation associated with it. Arthroscopy does possess certain unique aspects which need to be understood from the legal point of view as well. We obtained information on specific medico-legal cases involving arthroscopy from books and websites containing collections of medico-legal judgments in Indian legal courts, consumer dispute redressal forums at the state and national levels, and state medical councils. We assimilated and analysed all this information, combined it with our experience in the field of medical law, and have provided practical, enforceable ways to decrease the medicolegal risk for arthroscopy surgeons. This review provides a comprehensive overview of pressing issues in relation to the medicolegal aspects of arthroscopic surgery.
Legally Sound, Evidence-Based Informed Consent Form for Total Hip Arthroplasty
Informed consent documentation is often the first area of interest for lawyers and insurers when a medico-legal malpractice suit is concerned. However, there is a lack of uniformity and standard procedure for obtaining informed consent for total hip arthroplasty (THA). We aimed to develop a solution for this need for a pre-designed, evidence-based informed consent form for THA cases. We extensively reviewed the literature on the medico-legal aspects of THA, medico-legal aspects of informed consent, and medico-legal aspects of informed consent in THA. We then conducted semi-structured interviews with orthopaedic surgeons and patients who had previously undergone THA in the previous year. Based on all of the above, we developed an informed consent form that was evidence-based. We then had the form reviewed by a legal expert. The final form was utilised for THA cases at our institution for 1 year. Legally sound, evidence-based Informed Consent Form for Total Hip Arthroplasty is given in Form A. The use of legally sound, evidence-based informed consent for total hip arthroplasty cases would be beneficial to orthopaedic surgeons and patients alike. It would uphold the rights of the patient, and promote open discussion and transparency. In the event of a lawsuit, it would be a vital document in the defence of the surgeon and withstand the scrutiny of lawyers and the judiciary.
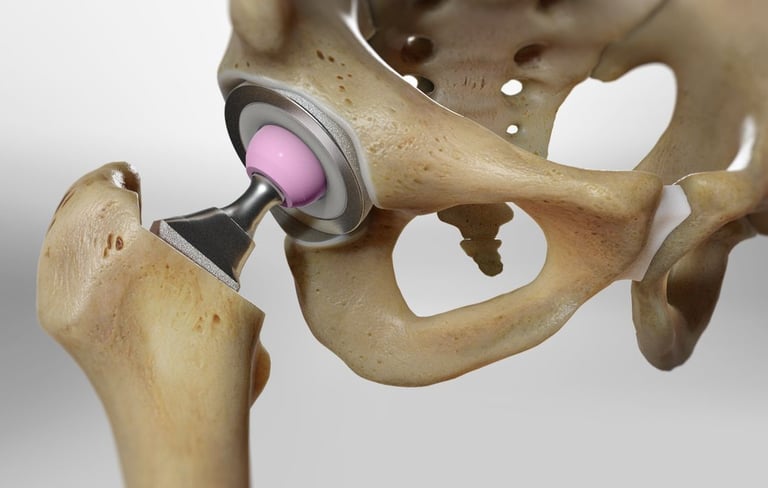
Medico-Legal Issues Related to Hip and Knee Arthroplasty: A Literature Review Including the Indian Scenario
Total hip arthroplasty (THA) and total knee arthroplasty (TKA) are commonly performed surgeries worldwide. The number of joint replacement surgeries being performed has increased considerably over the past two decades, but it has also seen an increase in litigation associated with it. The purpose of our study was to review and consolidate literature regarding medico-legal issues pertaining to THA and TKA cases. We looked at the causes of litigation, medico legal aspects of pre-operative requirements, optimisation of medical condition, indications and contraindications for arthroplasty, informed consent, implants, mixing of components from different manufacturers and post-operative rehabilitation. We also wanted to analyse available literature and legal proceedings regarding these cases in India specifically.
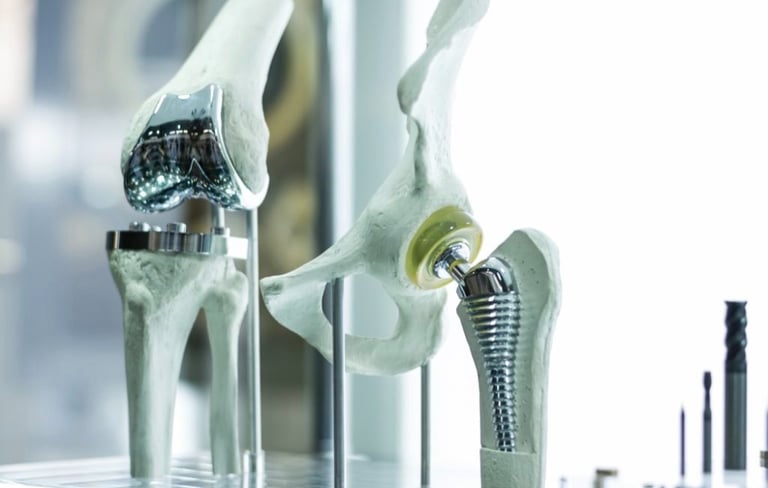
Malpractice or masterful practice? Navigating vicarious liability in healthcare
In the intricate landscape of healthcare, vicarious liability looms large, shaping the responsibilities and actions of healthcare practitioners and administrators alike. Illustrated by a poignant scenario of a medication error, this article navigates the complexities of vicarious liability in healthcare. It explains the legal basis and ramifications of this theory, emphasizing its importance in fostering responsibility, protecting patient welfare, and easing access to justice. The paper explores the practical effects of vicarious responsibility on day-to-day operations, leadership practices, and decision-making processes via the eyes of senior consultants, junior doctors, and hospital administrators. Through comprehensive insights and real-world examples, it underscores the imperative of fostering a culture of accountability, communication, and quality care to navigate the intricate web of liabilities inherent in modern healthcare.


The AI Orthopedician will see you now - But who is Liable if it's Wrong?
Artificial intelligence (AI) is revolutionizing various sectors, including health care, with orthopedics being no exception. Orthopedic practice, already familiar with technological advancements such as robotic surgery, is rapidly integrating AI into clinical workflows, enhancing precision in surgical planning, diagnostics, and patient care. However, this evolution raises critical questions, particularly regarding liability when AI systems fail and cause harm. This article delves into the role of AI in orthopedics, exploring its current applications and the potential legal implications that come with its adoption. It examines the global landscape, highlighting the lack of clear regulations around AI liability, especially in India, where the topic remains underexplored in medical literature. With insights into how AI is transforming orthopedic practice, the article addresses the pressing concern of who bears responsibility when AI errors occur. This timely discussion serves as an exploration of a unique and recent topic, urging Indian orthopedic surgeons to balance the benefits of AI with the responsibility they hold, as the legal framework surrounding AI in health care continues to evolve.


Evidence-based informed consent form for total knee arthroplasty
Informed consent documentation is often the first area of interest for lawyers and insurers when a medico-legal malpractice suit is concerned. However, there is a lack of uniformity and standard procedure about obtaining informed consent for total knee arthroplasty (TKA). We developed a solution for this need for a pre-designed, evidence-based informed consent form for patients undergoing TKA. We extensively reviewed the literature on the medico-legal aspects of TKA, medico-legal aspects of informed consent, and medico-legal aspects of informed consent in TKA. We then conducted semi-structured interviews with orthopaedic surgeons and patients who had undergone TKA in the previous year. Based on all of the above, we developed an evidence-based informed consent form. The form was then reviewed by a legal expert, and the final version was used for 1 year in actual TKA patients operated at our institution. Legally sound, evidence-based Informed Consent Form for Total Knee Arthroplasty. The use of legally sound, evidence-based informed consent for total knee arthroplasty would be beneficial to orthopaedic surgeons and patients alike. It would uphold the rights of the patient, promote open discussion and transparency. In the event of a lawsuit, it would be a vital document in the defence of the surgeon and withstand the scrutiny of lawyers and the judiciary.
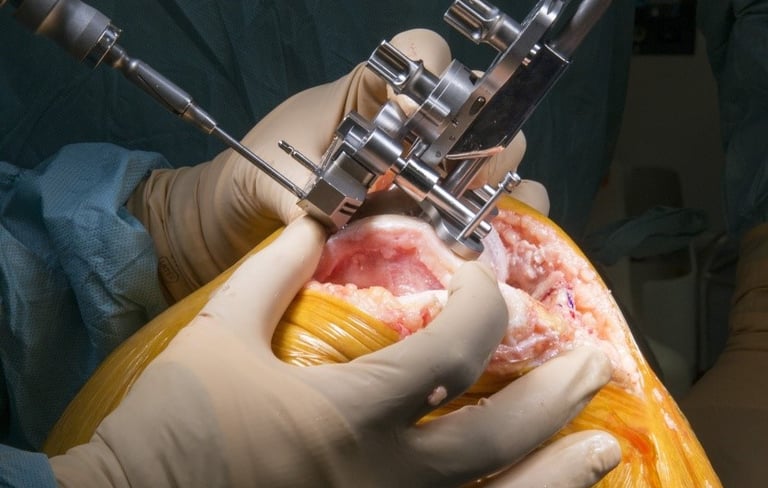
Beyond Blame: Is India Ready for No-Fault Liability in Healthcare?
In contemporary healthcare systems, the pursuit of justice intertwines with fault attribution and liability determination. The exploration of no-fault liability as a potential alternative within India's healthcare landscape delves into its feasibility and implications. Drawing from international experiences, regulatory frameworks, and societal readiness, the complexities and potential benefits of adopting a no-fault liability system are elucidated. Perspectives from patients, healthcare providers, and broader societal stakeholders are considered, highlighting both the advantages and challenges associated with such a transition. Addressing disparities in access, legal reforms, and logistical hurdles underscores the groundwork necessary for potential adoption, signaling a potential paradigm shift toward equitable compensation and accountability within India's healthcare system.


White Coats Under Fire: Understanding the Epidemic of Violence Against Doctors
The doctor-patient relationship, once grounded in trust and mutual respect, is increasingly marred by incidents of violence against healthcare providers. This alarming trend not only threatens the safety of doctors but also undermines the integrity of medical care. This article delves into the multifaceted reasons behind such violence, exploring emotional, financial, societal, and systemic factors that contribute to this disturbing phenomenon. Drawing from extensive surveys and real-world incidents, we shed light on the pressures and misunderstandings that fuel hostility towards medical professionals. Our analysis identifies key stressors, including heightened emotions, lack of understanding, financial burdens, societal prejudices, and systemic frustrations, which exacerbate tensions in healthcare settings. By understanding these underlying causes, we offer practical recommendations for doctors to navigate these challenges, emphasizing empathy, clear communication, and professional boundaries. Additionally, we highlight the need for systemic reforms, such as better security measures in hospitals and effective grievance redressal systems, to protect doctors and improve the overall healthcare environment. This article aims to raise awareness, foster dialogue, and provide actionable solutions to mitigate violence against doctors, ultimately striving to restore the sanctity of the doctor-patient relationship.


From Guidance to Grievance: Postgraduates, Mentors, and the Authorship Dispute
As a medical postgraduate, one is introduced into their field and has to get themselves up to terms with various aspects of clinical practice, apart from the theoretical aspects of the specialty. One such aspect that postgraduates have to familiarize themselves with during their course is research and publications. Research is an integral part of medicine, no matter which specialty one is practicing [1, 2]. As the world has moved clearly in the direction of evidence-based medicine, the medical literature is at the centerpiece of clinical decision-making. Literature, however, is an evolving entity. Research keeps advancing the field and helping medical professionals deliver better outcomes for their patients. This is why research has been identified as an essential part of postgraduate training. With research, comes the publication of that research work so that it reaches the clinicians and enables the entire medical fraternity and society to benefit from the research. The National Medical Council (NMC), identifying the importance of research and publications, has made it a compulsory requirement for all medical postgraduates to undertake a research study during their course, which needs to be written in the form of a thesis [3, 4]. This research work is to be carried out under the guidance of a postgraduate teacher termed the guide. This is an almost universal practice and is widely considered an important facet of postgraduate training. The problem, however, occurs when it comes to assigning credit for that research work during publication.



Guardian Med Legal Consulting
Medicolegal Support for Healthcare Professionals
Follow us
Based in Bangalore. Serving across India.
support@guardianmedlegal.com